Specialist Private BCG Vaccine & TB Testing in London | Book Online
Expert, specialist-led tuberculosis protection for infants, healthcare workers, and travellers at Hampstead Heath Pharmacy.
Private BCG Vaccination & Mantoux Testing in London
Protect your family, secure your career, and travel with confidence.
Hampstead Heath Pharmacy offers a specialist-led private TB (tuberculosis) vaccination and testing service. Whether you are a parent seeking protection for your infant, a healthcare worker requiring occupational clearance, or a traveller visiting high-risk regions, our clinic provides rigorous care in line with UK regulations and guidelines.
Licensed Vaccine
We exclusively use the BCG Vaccine AJV (Danish strain 1331)—currently the only BCG vaccine licensed in the UK and used by the NHS. We maintain strict cold-chain handling to ensure maximum efficacy.
Experienced Specialist
Vaccination is administered by our expert prescribing pharmacist, Mahyar Saremi, who brings over 10 years of experience in the precise intradermal technique required for BCG administration.
Integrated Testing
We offer on-site TB screening. Mantoux skin test results are read in 48–72 hours, and IGRA (TB blood test) results are returned in approximately 3 working days for fast clearance.
IMPORTANT: New Safety Requirement for Infants (SCID)
For all babies born on or after 1 September 2021, national safety protocols mandate that the BCG vaccine cannot be administered until the result of the Severe Combined Immunodeficiency (SCID) screening is confirmed negative. This screening is part of the routine newborn blood spot (heel prick) test performed at 5 days old.
- You must bring the Red Book to your appointment.
- You must bring the result letter confirming a negative SCID outcome.
Ready to secure your appointment? Book your BCG Vaccination, Mantoux Testing, or IGRA Blood Screen directly through our secure online portal.
Book Appointment Online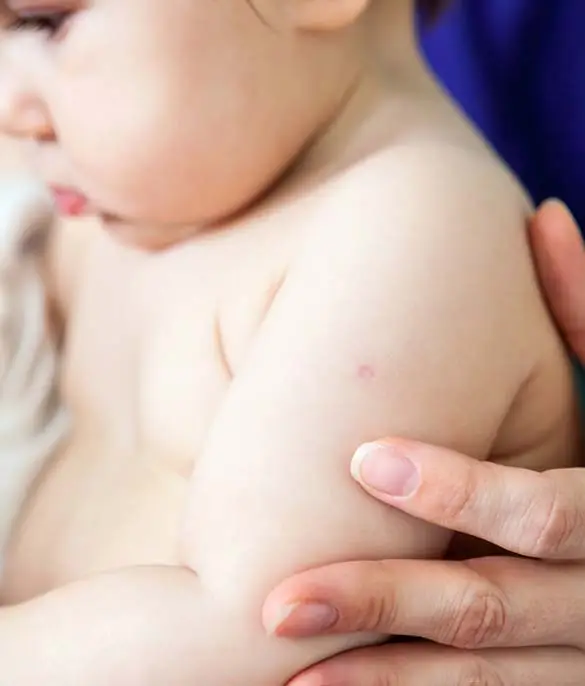
A message from the Mayor of London’s TB Ambassador, Emma Thompson, and her son Tindy on World TB Day
Why Consider the BCG Vaccine in London?
While the NHS transitioned to a targeted neonatal BCG programme in 2005, tuberculosis (TB) rates in London remain disproportionately high compared to the rest of the UK. Today, London accounts for roughly one in three of all TB cases in England.
Given the capital’s transient population and high mobility across boroughs, epidemiological models suggest an ongoing argument for universal vaccination to ensure a reliable safety net for children. For families seeking comprehensive protection outside the strict NHS criteria, our private service offers immediate access and peace of mind.
Patient Profile & Action Plan
Book BCG Vaccination. Must bring SCID results.
Book BCG Vaccination directly, unless the child has lived in a high-TB-prevalence country for >3 months (then book Mantoux first). Must bring SCID results.
Book Mantoux Test. Vaccination can only be done 48-72 hours after a negative result.
Do not book a vaccine. If you have a scar or record of previous BCG vaccination, repeat vaccination provides no additional protection. Book a Scar Check for evidence.
Employment & Travel Clearance
Occupational Health (NHS & Private Sector)
We support medical students, agency nurses, doctors, and care home staff who require evidence of TB immunity for employment clearance at our London clinic.- Compliance: Our certificates detail the date of administration, batch number (for vaccines), or millimetric induration reading (for Mantoux), satisfying standard Occupational Health audit requirements.
- Speed: We understand placement deadlines. Our streamlined service ensures you get your paperwork faster than standard NHS routes.
Professional Care, Transparent Costs
We believe in pricing integrity. The fees below are all-inclusive—no hidden “consultation fees” or “nurse access charges.”
| Service | Price | Includes |
|---|---|---|
| BCG Vaccination | £105 | Consultation, AJV Vaccine, and Aftercare advice. |
| Mantoux Test | £85 | Administration AND the follow-up reading appointment (48-72hrs). |
| TB Blood Test (IGRA) | £144 | Phlebotomy (blood draw) and laboratory analysis with report. |
| BCG Scar Check | £40 | Clinical inspection and Certificate of Verification. |
| Replacement Certificate | £15 | Re-issue of lost documentation. |
Note: If a Mantoux test is required before vaccination, it is charged as a separate procedure (£85 + £105) due to the multiple appointments involved and the test cost.
Before You Book: The “4-Week Rule”
To ensure your appointment proceeds smoothly, please verify the following regarding MMR Vaccines:
Have you or the patient received an MMR (Measles, Mumps, Rubella) vaccine in the last 4 weeks?
Clinical Rule: A Mantoux test cannot be performed within 4 weeks of an MMR vaccine, as the live virus can cause a false negative TB result. Please schedule your appointment after this 4-week window has passed.

Expert Answers
Why is the BCG vaccine given in the left arm?
By convention, the BCG is administered in the upper left arm to make it easier for healthcare professionals to locate the scar for verification later in life.
What should I expect after the BCG vaccination?
A small red spot usually appears within 2–6 weeks, which may develop into a blister or pustule. This is normal and indicates the vaccine is working. It heals to leave a small scar. Do not squeeze or apply plasters to the site (unless swimming).
Why can’t I get a BCG vaccine on the NHS?
The NHS stopped universal BCG vaccination in 2005, and it is now only offered to those considered high risk by local health authorities. However, recent UKHSA reporting shows that TB incidence has been increasing in England, particularly in large urban areas like London. Because many families do not qualify for NHS vaccination or face long waiting lists, our private clinic provides immediate, accessible protection.
Is the Mantoux test painful?
It involves an intradermal injection — a small scratch under the top layer of skin. It creates a temporary bleb that disappears quickly. Most patients describe it as a brief sting.
How much does a private BCG vaccination cost in London?
At Hampstead Heath Pharmacy, a private BCG vaccination costs £105 all-inclusive — covering the consultation, the AJV vaccine, and aftercare advice. No hidden fees. If a Mantoux test is required beforehand, it is an additional £85.
Do I need a Mantoux test before BCG vaccination?
Yes, for all individuals aged 6 years or older. Children under 6 only require a Mantoux test if they have lived in or visited a high-TB-prevalence country for more than 3 months, or have had close contact with someone with active TB.
What is the difference between a Mantoux test and an IGRA blood test?
Both screen for TB exposure, but work differently. The Mantoux test involves injecting tuberculin under the skin and reading the result 48–72 hours later (two visits required). The IGRA (QuantiFERON) is a blood test that requires only a single visit, with results available in about 3 working days. Crucially, the IGRA is not affected by previous BCG vaccination, making it ideal for anyone who has had BCG before.
The deposit paid at the time of booking an appointment will be deducted from the total service cost when you visit us, provided you adhere to our cancellation policy.
Ready to Book?
Secure your private BCG vaccination or TB testing appointment at our London clinic using the portal below.
Need a home visit instead? Email our team directly.
For BCG Vaccines, Mantoux Tests, or Scar Verifications: Please select a "Non-Travel Vaccination Appointment" from the menu.
For TB Blood Tests (IGRA): Please select a "Blood Testing Appointment" from the menu.
Important Note: The deposit paid at the time of booking is not an extra fee. It is fully deducted from your total service cost on the day of your visit, provided you adhere to our cancellation policy.
Mahyar SaremiSuperintendent Pharmacist Prescriber
GPhC Registration: 2069409
Last reviewed: April 2026 | Next review due: April 2027
